In many parts of the world, long weekends are planned months in advance. Flights are booked, cabins reserved, routes mapped. Families coordinate schedules and look forward to a brief pause from everyday routines. And then, sometimes at the very last minute, the weather intervenes.
A heatwave cancels outdoor plans. Wildfire smoke grounds flights. Flooding closes highways. A hurricane shifts course. In other cases, it’s the opposite — a late-season snowstorm shuts down airports, buries roads, and leaves everyone asking how this fits into a “warming planet.” What was meant to be a brief escape turns into a scramble to reroute, reschedule, or simply stay home.
For most of us, this registers as an inconvenience. A ruined vacation. A wasted reservation. An unexpected expense. We may grumble, post a photo of grey skies or flight delays, and move on.
If you are reading this article at any point in time — whether this year or should time travel become a thing—from the future (and hopefully still on Planet Earth), chances are your family has experienced at least one such disruption. These moments have become common enough that they barely register as unusual.
They also tend to spark a familiar question: If the planet is warming, why is it still snowing?
But pause for a moment and widen the lens and this is where the distinction between weather, climate change, and global warming matters. Weather describes short-term events—a snowstorm, a heatwave, a heavy rain. Climate change refers to long-term shifts in patterns, intensity, and variability. Global warming refers specifically to the long-term increase in average global temperatures, which can destabilize atmospheric systems and, paradoxically, lead to more extreme cold events in some regions.
Organizations such as the World Health Organization (WHO), the Centers for Disease Control and Prevention (CDC), and the United Nations have consistently emphasized this distinction. Climate change does not eliminate cold or snow; it makes weather more unpredictable, more intense, and more disruptive.
And while these disruptions may feel minor in our daily lives, they are often the first visible signals of a much larger system under stress — one with implications that extend far beyond a single long weekend.

From Inconvenience to Catastrophe
Climate change does not affect everyone equally. The storm that cancels a beach trip in one country may erase an entire community in another. The heatwave that keeps a city indoors for a few days may prove fatal elsewhere.
In many developing and underdeveloped regions, climate-related events are not temporary disruptions — they are existential threats. Floods contaminate drinking water and spread disease. Droughts collapse food systems and livelihoods. Extreme heat overwhelms already fragile health infrastructure, leaving hospitals understaffed, underpowered, or inaccessible when they are needed most.
Recovery in these contexts is rarely quick. It is often slow, incomplete, or impossible. What appears elsewhere as a short-term inconvenience becomes, for millions of people, a long-term health crisis.
This disparity is central to understanding climate change as a health issue, not just an environmental one. Health risks multiply where systems are weakest, resources are scarce, and safety nets are thin. Climate shocks interact with poverty, inequality, and limited access to care, amplifying their impacts on physical and mental health.
Importantly, these outcomes are not hypothetical. They are already unfolding. Rising temperatures are increasing heat-related illness and mortality. Changing precipitation patterns are driving food and water insecurity. Shifts in ecosystems are expanding the range of infectious diseases. Healthcare systems — particularly in vulnerable regions — are being stretched beyond capacity.
It is in this context that global health institutions increasingly describe climate change not as a future concern, but as an ongoing humanitarian and public health emergency — one that threatens to reverse decades of progress in global health and development if left unaddressed.
Climate Change as a Global Health Emergency: What Institutions Are Saying
Climate change is no longer framed by leading institutions as a distant environmental concern. It is increasingly understood as a global health emergency—one that threatens lives, strains health systems, and undermines decades of progress in public health and development.
This shift is evident in how major organizations approach climate change today.
World Health Organization (WHO): Climate Change as a Threat Multiplier
The World Health Organization has been unequivocal: climate change is one of the greatest health threats facing humanity. WHO describes it as a “threat multiplier”—one that intensifies existing health challenges while creating new ones.

According to WHO:
- 3.6 billion people already live in regions highly vulnerable to climate change
- Between 2030 and 2050, climate change is expected to cause approximately 250,000 additional deaths per year from heat stress, undernutrition, malaria, and diarrheal disease alone
- Regions with weak health infrastructure, largely in developing countries, are least able to cope without significant external support
WHO also emphasizes that climate action is a health opportunity. Reducing greenhouse gas emissions—particularly through cleaner energy, better transport, and improved food systems—can deliver immediate health benefits, most notably through improved air quality and reduced pollution-related disease.
Centers for Disease Control and Prevention (CDC): A Public Health Lens
In the United States, the CDC frames climate change as a growing public health stressor that amplifies existing risks and introduces new ones.
The CDC identifies climate-sensitive health risks including:
- Increased respiratory and cardiovascular disease linked to air pollution
- Injuries, illness, and premature deaths associated with extreme heat and weather events
- Shifts in food-, water-, and vector-borne diseases
- Mental health impacts, including stress, anxiety, trauma, and displacement
Importantly, the CDC highlights that vulnerability is not uniform. Age, income, geographic location, housing quality, and access to healthcare all influence who is most at risk—reinforcing that climate change is as much a social and equity issue as it is a physical one.
World Bank: Health, Climate, and Economic Stability
The World Bank approaches climate change through the interconnected lenses of health, poverty, and economic resilience. It has described climate change as a global health emergency with consequences of historic scale.
Key findings include:
- Climate change could result in at least US$21 trillion in excess health-related costs in low- and middle-income countries by 2050
- Without action, climate impacts could push 132 million people into extreme poverty by 2030, with more than half of that increase driven by health-related factors
The World Bank also notes a critical feedback loop: while health systems are highly vulnerable to climate change, the health sector itself contributes approximately 5% of global greenhouse gas emissions, underscoring the importance of decarbonizing healthcare infrastructure alongside strengthening resilience.
How Climate Change Impacts Health
Taken together, the perspectives of WHO, CDC, and the World Bank point to a shared conclusion: climate change affects health through multiple, interconnected pathways. Some risks intensify, others emerge, and none are evenly distributed.
As illustrated in the climate–health framework above, climate change influences health both directly and indirectly, shaped by exposure, vulnerability, and system capacity.
Key pathways include:
- Air pollution
- Increased exposure to fine particulate matter and ozone
- Higher rates of asthma, cardiovascular disease, and respiratory illness
- Temperature extremes
- Heat-related illness, heat stroke, and increased mortality
- Disproportionate impacts on older adults, children, outdoor workers, and pregnant individuals
- Precipitation extremes
- Flooding and drought that disrupt water quality and sanitation
- Increased risk of waterborne disease
- Food security and nutrition
- Reduced food availability, quality, and diversity
- Increased undernutrition and foodborne illness
- Vector-borne diseases
- Expansion of mosquitoes, ticks, and other vectors
- Increased transmission of diseases such as malaria and Lyme disease
- Mental health and psychosocial impacts
- Anxiety, trauma, and stress related to displacement, loss, and uncertainty
- Long-term mental health consequences following climate disasters
These impacts are mediated by social, economic, and environmental determinants—meaning that communities already facing inequities experience the greatest harm.
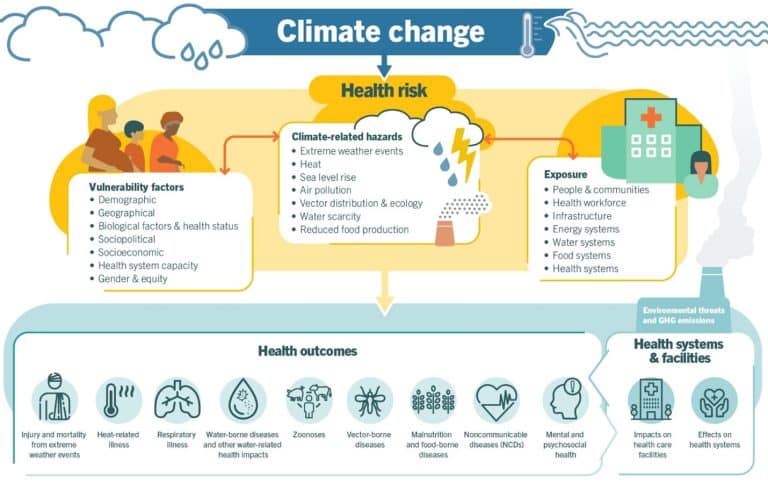
Figure: Overview of climate-sensitive health risks, including exposure pathways and vulnerability factors. Climate change affects human health both directly and indirectly, with impacts strongly influenced by environmental, social, and public health determinants.
Source: U.S. Centers for Disease Control and Prevention (CDC).
Why this framing matters
When climate change is understood primarily as an environmental issue, responsibility feels distant and abstract. When it is understood as a health emergency, the implications become immediate, personal, and ethical.
It was against this growing recognition—during a moment when global health systems were already under extraordinary strain—that I hosted a conversation on climate change and health in 2020. That discussion, and what followed, helped crystallize why health must sit at the center of climate action.
When Climate Change Becomes Personal: A Health Perspective
Reflections on why climate change is, and will remain, a human health issue
This article is written in early 2026, reflecting on a conversation hosted several years earlier. If you are reading this in 2035 or 2040, the science discussed here may have evolved. However, the central premise has not changed: climate change is not only an environmental or technical challenge. It is fundamentally a human health issue. That reality has only become more evident with time.
Why this conversation still matters
In late 2020, as much of the world was emerging from the acute phase of the COVID-19 pandemic, I moderated a webinar on Climate Change and Health. The speakers were Dr. Joan Schiller, a medical oncologist, and her son, Craig Schiller, a climate and green building professional.
At the time, climate change was already well understood scientifically, yet it was still often discussed in abstract terms—emissions curves, temperature thresholds, and distant future impacts. Framing climate change through the lens of human health made the issue immediate, personal, and difficult to ignore.
Since then, extreme heat events, wildfire smoke, air quality alerts, healthcare system strain, and climate-driven displacement have become more visible and more frequent. What felt like an emerging perspective in 2021 now feels unavoidable. That is why this conversation—and the insights that emerged from it—remain deeply relevant today.
Why I hosted this discussion in the first place
During the pandemic, GBRI hosted numerous webinars addressing sustainability, resilience, and post-COVID strategies. This particular session was not initially intended to launch a broader initiative. It was simply an attempt to explore climate change from a different angle—one rooted in lived experience and human vulnerability.
Inviting a physician into a climate discussion was intentional. We wanted to move beyond technical metrics and ask a more fundamental question:
What does climate change actually mean for human health—across a lifetime?
The response to that question exceeded expectations. The conversation resonated not only because of the science, but because it connected climate change to things people care about deeply: family, community, safety, and well-being.

A doctor’s lens: climate change as a public health issue
Dr. Schiller approached climate change not as an environmental advocate, but as a physician who had spent decades treating patients and studying disease. One of her most compelling observations was how closely climate change mirrors chronic illness:
- It develops slowly
- Early warning signs are often ignored
- The most severe consequences appear years later
- Prevention is far more effective than treatment
From a medical perspective, human health depends on clean air, safe water, reliable food systems, access to healthcare, and social stability. Climate change disrupts all of these simultaneously. When framed this way, climate change stops being an abstract environmental concern and becomes a direct public health challenge.
How climate change shows up in the human body
One of the strengths of the 2020 discussion was how clearly it traced environmental change to physical health outcomes—not hypothetically, but measurably.

Key climate change impacts on human health
(Synthesized from the expert discussion available on GBRI, USGBC and Youtube)
- Extreme heat
- Increased risk of heat exhaustion, heat stroke, and cardiovascular stress
- Higher risks for children, older adults, outdoor workers, and pregnant individuals
- Air pollution
- Increased exposure to fine particulate matter (PM2.5) and ozone from fossil fuel combustion and wildfires
- Links to asthma, respiratory disease, cardiovascular illness, and lung cancer
- Vector-borne diseases
- Expansion of mosquito and tick ranges due to warming temperatures
- Increased incidence of diseases such as Lyme disease and malaria
- Healthcare system disruption
- Climate-driven disasters strain hospitals and emergency services
- Delayed preventive care and treatment during extreme events
Together, these pathways reveal a critical insight: climate change affects not only ecosystems, but human bodies.
COVID-19 as a case study in system fragility
COVID-19 was not caused by climate change, but it offered a powerful illustration of what happens when complex systems are overwhelmed. Healthcare shortages, disrupted supply chains, delayed treatment, and mental health strain highlighted the fragility of systems many assumed were resilient.
Climate-related disruptions—whether heat waves, floods, hurricanes, or wildfires—place similar pressures on healthcare and social infrastructure, often repeatedly and unpredictably. From a health perspective, the lesson is clear: resilience is essential, not optional.
The built environment connection
Craig Schiller’s contribution helped connect health outcomes directly to buildings and infrastructure. Buildings influence indoor air quality, thermal comfort, exposure to pollutants, and energy use—often on a daily basis.
Choices related to fuel sources, ventilation, envelope design, and material selection have measurable health implications. Climate action, therefore, is not only about reducing emissions; it is also about improving the environments where people live, work, learn, and heal.
This realization helped catalyze broader educational efforts within GBRI, including the development of climate skills training and the Climate Change Ambassador Program.

What this means for architects, designers, builders, and planners
Professionals shaping the built environment play a critical role in addressing climate-related health risks. Buildings and infrastructure are not neutral—they influence daily exposure to heat, air pollution, noise, water quality, and system reliability. Thoughtful design and construction decisions can either amplify health risks or significantly reduce them.
Key considerations include:
- Indoor air quality and ventilation
Building design directly affects exposure to particulate matter, volatile organic compounds (VOCs), and combustion byproducts. Adequate ventilation, filtration, and source control are essential for protecting occupant respiratory and cardiovascular health. - Fuel choices and combustion sources
The choice between fossil fuel–based systems and all-electric alternatives has measurable health implications. Reducing on-site combustion lowers exposure to nitrogen dioxide (NO₂), carbon monoxide, and ultrafine particles, particularly in residential and high-occupancy spaces. - Passive survivability during extreme heat or outages
As heat waves and power disruptions become more frequent, buildings must be able to maintain safe indoor conditions without full mechanical systems. Passive design strategies can be lifesaving during extreme events. - Material selection and exposure reduction
Materials influence both embodied emissions and indoor environmental quality. Low-emitting, durable materials reduce long-term exposure risks while supporting healthier indoor environments. - Resilience to climate-driven disruptions
Flooding, heat, storms, and supply chain disruptions increasingly affect building operations. Designing for resilience helps protect both physical assets and human health over the life of a project.
Understanding these connections is increasingly part of responsible professional practice.
Practical actions professionals can take

For architects, designers, and planners
- Prioritize location and siting decisions
Where a building is located directly affects exposure to flooding, extreme heat, wildfire smoke, and sea-level rise. Avoiding high-risk areas and incorporating climate-informed site analysis reduces long-term health and safety risks. - Design for access to transportation and essential services
Proximity to public transportation, healthcare, food access, and community services influences both daily health outcomes and emergency response during climate events. - Incorporate climate-resilient and adaptive design strategies
Designing for future climate conditions—rather than historical baselines—helps protect occupants from increasing heat, storms, and infrastructure stress. - Prioritize all-electric or low-combustion building systems
Electrification reduces both operational emissions and indoor air pollutants, improving long-term respiratory and cardiovascular health.
- Design for enhanced ventilation, filtration, and indoor air quality
High-performance ventilation and filtration reduce exposure to pollutants and airborne pathogens, especially during smoke events and heat waves. - Incorporate passive cooling and survivability strategies
Shading, natural ventilation, thermal mass, and envelope optimization support safe indoor conditions during extreme heat or power outages. - Reduce indoor sources of air pollution through material selection
Low-emitting, durable materials reduce long-term exposure risks while supporting healthier indoor environments.
For builders and contractors
- Implement best practices for indoor air quality during construction
Protecting ductwork, controlling dust, and managing moisture improves post-occupancy health outcomes. - Minimize on-site combustion where feasible
Reducing diesel equipment use lowers exposure to nitrogen dioxide and particulate matter for workers and nearby communities. - Reduce embodied carbon through material and procurement choices
Selecting lower-carbon materials and optimizing construction processes reduces upstream emissions that contribute to air pollution and climate-related health impacts. - Educate clients on healthier operational and maintenance choices
Contractors play a critical role in translating design intent into real-world performance and health outcomes.

For owners and operators
- Monitor indoor air quality
Ongoing monitoring enables early detection of issues related to ventilation, filtration, and pollutant sources. - Improve ventilation in kitchens and high-use areas
Targeted ventilation reduces exposure to combustion byproducts and cooking-related pollutants. - Plan for heat resilience and emergency preparedness
Operational planning for extreme heat, smoke events, and outages protects occupants during increasingly common disruptions. - Integrate climate risks into operations and maintenance planning
Anticipating heat events, smoke days, and power disruptions helps protect occupants and maintain continuity of care, work, and daily life.
How green building rating systems address climate change, equity, and health

Green building and infrastructure rating systems provide structured, measurable frameworks for addressing the interconnected challenges of climate change, human health, and equity. They help translate broad goals into actionable project requirements.
LEED (Leadership in Energy and Environmental Design)
LEED addresses climate and health through energy performance, indoor environmental quality, material selection, and resilience strategies. The latest evolution of LEED emphasizes impact-driven outcomes, including:
- Decarbonization – Reducing operational and embodied carbon emissions
- Quality of life – Improving indoor environmental quality, thermal comfort, and occupant well-being
- Ecological Restoration – Protecting natural systems and supporting long-term environmental resilience
These impact areas explicitly connect climate action with human health and community outcomes.
WELL Building Standard
The WELL Building Standard places human health and well-being at the center of design, construction, and operations, explicitly recognizing that buildings are a primary interface between people and the changing climate.
WELL addresses climate–health connections through features related to air quality, thermal comfort, water, nourishment, mental health, and equity, all of which are increasingly affected by climate change. As climate-related stressors intensify—such as extreme heat, poor air quality, water scarcity, and displacement—WELL prioritizes strategies that help protect both physical and mental health in indoor environments.
According to the International WELL Building Institute (IWBI), climate change represents one of the greatest challenges to human health, with disproportionate impacts on vulnerable populations. WELL’s framework emphasizes not only environmental performance, but also human-centered resilience, encouraging spaces that support recovery, stress reduction, and long-term well-being in the face of climate disruption.
By integrating health equity, occupant experience, and climate-responsive design, WELL complements other sustainability frameworks such as LEED by ensuring that decarbonization and resilience efforts translate into measurable improvements in quality of life, particularly for those most affected by climate-related risks.
Envision (Sustainable Infrastructure Framework)
For infrastructure projects, Envision provides a complementary framework that integrates sustainability, resilience, equity, and public health considerations at a systems level. Envision encourages:
- Climate-resilient infrastructure design
- Reduced emissions across project lifecycles
- Protection of community health and well-being
- Inclusive decision-making and equitable outcomes
Together, these frameworks help align building and infrastructure projects with global climate and health goals while addressing the needs of diverse communities.

From one conversation to climate skills development
In hindsight, the 2020 webinar marked an inflection point. It helped inspire the creation of more comprehensive climate education offerings. The goal shifted from awareness to capacity—empowering professionals across disciplines to understand climate risks, communicate them effectively, and contribute to solutions.
A reason for cautious optimism
Not every day—or every long weekend—will go as planned in a changing climate. Weather will continue to disrupt routines. Heat waves, storms, smoke, and flooding will test systems and communities. But alongside these challenges, meaningful progress is underway.
In the built environment, new frameworks and leadership are reshaping how climate action and human health are addressed. LEED v5, for example, places impact at the center of its approach, with clearly defined focus areas including decarbonization, quality of life, and ecosystems. This shift reflects a broader recognition that sustainability is not only about efficiency, but about outcomes that directly affect people and communities.
At the same time, corporations across sectors are increasingly using LEED and the WELL Building Standard to advance environmental, social, and governance (ESG) goals. These frameworks are helping organizations translate climate commitments into healthier workplaces, lower-emission operations, and more equitable environments—connecting climate action with employee well-being, productivity, and long-term resilience.
Cities and governments are also playing a growing role. From heat action plans and climate-resilient infrastructure to improved public transportation and community preparedness strategies, public-sector leadership is helping communities anticipate and adapt to climate risks. While no system is immune to disruption, these efforts are strengthening the capacity to respond, recover, and protect human health.

This is where hope resides—not in the absence of risk, but in the growing alignment between climate science, health priorities, and professional practice. Progress may be uneven, and setbacks are inevitable. Yet the tools, knowledge, and frameworks available today are far more advanced than they were just a few years ago.
If a long weekend goes wrong, it may still be frustrating. Plans may still change. But increasingly, buildings, infrastructure, and communities are being designed with the understanding that disruption is not an exception—it is a condition we must plan for.
Climate change is becoming personal because it touches daily life. It is also becoming actionable, as professionals across disciplines step into their role in protecting health, strengthening resilience, and shaping a more sustainable future.

An invitation to go deeper
This article offers a synthesis and reflection on the themes discussed. For those who wish to hear directly from Dr. Joan Schiller and Craig Schiller, the full 1.5-hour Climate Change and Health video course is available through the GBRI and USGBC platforms, as well as in public domains such as YouTube, and continues to resonate with learners across disciplines.
Continue Your Journey: Explore the Course Between Climate & Health

Climate Change And Health: A Lunchtime Chat With Dr. Joan Schiller
Dr. Joan Schiller is a medical oncologist and adjunct professor at University of Virginia. She is passionate about the impact of climate change on health. She recently published two articles on the subject in The Journal of Clinical Oncology – Oncology Practice and Lung Cancer News, a publication of the International Association for the Study of Lung Cancer.
Join us as Dr. Schiller explores the topic and shares her wisdom.
Centers for Disease Control and Prevention. (n.d.). How climate change affects health.
https://www.cdc.gov/climate-health/php/effects/index.html
Global Burden of Disease Study Collaborators. (2023). The health effects of climate change: A global perspective. International Journal of Environmental Research and Public Health, 20(4), Article 3160.
https://pmc.ncbi.nlm.nih.gov/articles/PMC10016220/
GBRI. (n.d.). Climate change and health: A lunchtime chat with Dr. Joan Schiller and Craig Schiller [Video course].
https://www.gbrionline.org/courses/climate-change-and-health-a-lunchtime-chat-with-dr-joan-schiller-craig-schiller/
Institute for Sustainable Infrastructure. (n.d.). Use Envision.
https://sustainableinfrastructure.org/envision/use-envision/
United Nations Development Programme. (n.d.). Climate change and health.
https://www.adaptation-undp.org/climate-change-and-health
U.S. Green Building Council. (n.d.). Building decarbonization to combat climate change.
https://www.usgbc.org/articles/building-decarbonization-combat-climate-change
World Bank. (n.d.). Health and climate change.
https://www.worldbank.org/en/topic/health/brief/health-and-climate-change
World Health Organization. (n.d.). Climate change and health.
https://www.who.int/news-room/fact-sheets/detail/climate-change-and-health
International WELL Building Institute. (n.d.). Climate change and human health: Doubling down on our planet’s greatest challenge.
https://resources.wellcertified.com/articles/climate-change-and-human-health-doubling-down-on-our-planets-greatest-challenge/






